General considerations, indications, and potential advantages of chest wall stabilization, rib fixation, and sternum osteosynthesis in selected patients after blunt trauma
Rib fractures
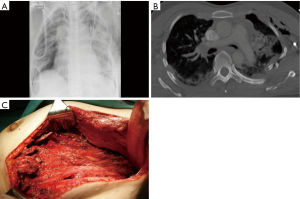
The treatment of rib fractures associated with blunt chest wall trauma is still commonly conservative. However, conservative management can be associated with complications in the acute phase following the trauma, due to its duration or to its inefficacity (1,2). Most usual complications consisted of infections and prolonged respiratory failure, leading to extended hospitalization and high mortality rate. It should be mentioned that mortality rate is not only associated with the thorax trauma itself but is also strongly dependent on other injuries, age and comorbidities. Several reports have shown that conservatively treated rib fractures can often be accompanied by impairment of the daily activity and of the quality of life, due to persistent pain or chest wall deformity, fracture nonunion, chest tightness (1-3). Bhatnagar observed a loss of an average of 70 days of work during recovery after conservative therapy of flail chest (2), Landerscaper described a long-term disability in up to 60% of the patients (3). In the last years, an increasing interest for stabilization of the chest wall in flail chest patients or for rib fixation has considerably raised. This was underlined by the development of new surgical fixation devices and the creation of several courses on chest wall surgery in order to make the indications and the techniques more familiar to the surgical community. This is a very important point since rib fractures are still often banalised and their long-term consequences underestimated. Indeed, many surgeons do not pay much attention on rib fractures and are unfamiliar with the indications and fixation techniques. Moreover, the level of evidence of the published data is relatively low, due to the heterogeneity of the indications for surgery, of the techniques used, and to the relatively small number of patients included. An often mentioned argument in favor of conservative management of rib fractures is the absence of solid data from prospective, randomized trials showing clear advantages for the patients after surgical fixation. The question is: do we really need such prospective randomized trials? I think it is not necessary because there are data from small prospective randomized trials, systematic reviews and meta-analysis or from other monocentric studies showing that early stabilization in flail chest can improve incidence of pneumonia, need for tracheostomy, duration of intubation, length of intensive care unit and hospital stay in comparison with conservative therapy (4-12). Moreover, for a surgeon who is experienced with the procedure and who is convinced of the potential positive results of the operation in selected patients with flail chest, the process of randomization would probably be not possible in many cases. Figure 1 gives an example of such a situation. A prospective, randomized study should include all the patients with flail chest potentially operable after exclusion criteria. For me, it would be impossible to randomize the young woman described in figure 1 and to risk offering her a prolonged conservative therapy. It is anyway true that there is a lack of solid data regarding the long-term results on functional outcome, pain control, quality of life, and survival. Such analysis could be assessed by comparing the results of large experienced centers treating the patients either conservatively or surgically rather than by a prospective randomized study design. Some prospective monocentric studies have described a positive long-term outcome after rib fixation in patients with flail chest with a return to work rate at 2 months of 100% with a 95% to 100% working capacity, no restriction in lung function test at 6 months (13,14). Majercik observed no residual pain after fixation already 5.4 weeks postoperatively with a mean satisfaction score of 9.2 on visual scala (10). A recent retrospective single institution study with an acceptable number of included patients showed a statistically significant proportion of patients with less pain and a return to normal activity after operative management than after conservative therapy (15).
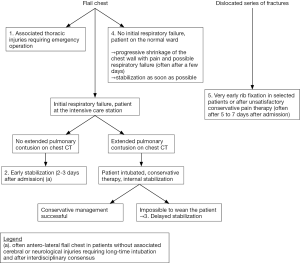
The selection of the patients who should undergo rib fixation is an extremely important step. This selection requires a well-established cooperation between emergency station, traumatology, and thoracic surgery units. It is a considerable advantage if thoracic surgeons are early involved, due to the relatively high incidence of associated intrathoracic injuries but also to reach a rapid consensus immediately at admission at the emergency unit or latest at the intensive care unit. In most of the cases, the situation will be discussed 1 or 2 days after admission again. An interdisciplinary plan of the management of the patients should be given, according to the associated injuries. Regarding to the indications to surgical stabilization of the chest wall or to rib fixation, 5 situations can be pointed out (Figure 2). First, patients with flail chest presenting with associated thoracic injuries requiring immediate surgery (haemothorax with persistent bleeding and hemodynamically instable patient, diaphragm or heart injuries). Second, patients with severe flail chest (mostly antero-lateral) with respiratory failure but without cerebral injuries require a prolonged intubation time. These patients should be operated as soon as possible if severe lung contusion (from 30% of the lung) is absent. We should be aware that the complete extension of lung contusion is mostly visible about 2 days after trauma, which usually leads to renew chest CT. This group of patients should be operated as soon as possible, generally 2 or 3 days after admission to avoid pneumonia, which could ruin the potential advantages of the operation. In most of the cases (90%), extubation is possible immediately after operation or in the first 24 hours (1). If extended lung contusion is present, early operation should be avoided, since complication rate is high and the patients can not benefit from the operation in term of early mobilisation (16). A special absolute indication for stabilization in this subgroup consists of patients presenting with bilateral parasternal fractures (costochondral separation), often resulting from cardiac reanimation. The sternum itself is the instable segment of the chest wall. A third indication consists of patients with severe flail chest with extended lung contusion requiring prolonged intubation. These patients can be operated later (often after 2, 3 weeks) if the weaning procedure is difficult. A fourth indication is observed in patients without initial respiratory failure. Most of these patients have been transferred on the normal ward with an adapted pain therapy. After a few days to 10 days, a progressive shrinkage of the chest wall is observed with increase of pain or respiratory failure.
In the last years, indication for rib fixation was also extended in selected patients without flail chest. These patients suffer from multiple dislocated and painful rib fractures. Small series recently published suggest that patients benefit from the rib fixation in terms of pain control and functional results but there is no long-term outcome in these articles (7,14,15). Again, I also think that there is no absolute need for prospective randomized studies comparing conservative with surgical therapy in this subgroup of patients. The true question is not any more if a treatment is superior to the other one but to be able to select patients who can benefit from an operation. It is clear that not all patients with multiple rib fractures should undergo fixation. In my opinion, there are 2 subgroups of patients who should be relatively early operated. First, young active and sporty patients who wish to be fit as soon as possible again and second, older patients who are living alone, independently and are still active with a good quality of life. In such patients, operations should be proposed early at admission or after some days. For the other patients, an adequate pain therapy should be initiated and optimized up to 1 week, consisting of different possible combinations of oral drugs, PCA (patient controlled anesthesia)-pump or peridural analgesia. Rib fixation should be offered in patients with persisting pain and dislocated ribs.
Special attention should be given during initial physical examination in order to correctly diagnose multiple rib fractures associated with dislocation of the costal arch. This dislocation is not always easy to notice and if several ribs are fractured, this situation leads to an instability. If only the ribs are fixed without reparation of the costal arch, shearing forces with rotation component will usually result in persisting pain, deformity and eventually to fractures or dislocation of the material. Reconstruction of the costal arch should be always performed, avoiding injury of small branches of intercostal nerves which could lead to an invalidating relaxation of a part of the superficial abdominal musculature.
Regarding to the technique used for rib fixation, several devices are available (Figure 3). The choice of the material used depends on the localization of the fractures, of the quality of the bone and also of the own experience of the surgeon. The technique should be fast and as atraumatic as possible. Care should be taken to avoid to injuring the contused soft tissue. Ribs should not be denuded and attention should be given to the intercostal bundle. This point is of paramount importance, since injuries of the intercostal structures during operation often lead to disabling chronic pain. The majority of the modern devices are made of titanium, which allows optimal adaptation to the anatomy of the ribs and ensures good protection against infection. Systems with plates and screws can be used in each parts of the ribs and allow an optimal reposition of the fractures. These systems might be sometimes time consuming and be rather reserved for difficult situations and reconstruction of the costal arch. They can usually be used in cartilage too. Other techniques using screwless systems have the advantage to be quick. They can be applied through smaller incisions which protect the contused soft tissue. Through the same incisions, 3 to 4 ribs can be fixed. These system scan also be used in osteoporotic bones. However, ruptures of the material have been described, leading sometimes to reoperation in the case of pain or instability of the chest wall (17). Another system, consisting of nitinol (alloy of titanium and nickel) has been recently introduced. This system is based on thermic properties, since the material is malleable in cold water. After application on the fracture, simple contact with a warm dress allows return in the initial hard position, giving stability.
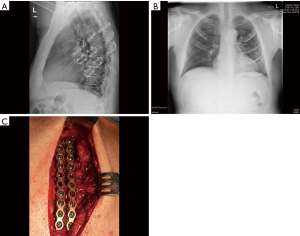
Is it necessary to fix all the fractured ribs? The first two ribs do not need to be stabilized. In the case of associated fractures of the first rib and of the clavicle, then the clavicle should be operated to avoid instability of the shoulder girdle. Fixation of all the fractures is probably not necessary. However, care should be taken to avoid persistent deformity of the chest wall, leading to possible functional restriction. Generally, after reposition of the most dislocated fractures, the other fractures automatically take a normal alignment.
Does rib fixation lead to stiffness of the chest wall? Stiffness of the chest wall is described in about 15% to 20% of the patients after blunt trauma, independently of the type of material used for fixation (1). Several reports suggest that stiffness is rather a consequence of the trauma itself than of the operation (1,10). Indeed, lung function testing at 6 months has not revealed any restriction in these observations and our experience has shown that removal of the material does not lead to any improvement in most of the cases.
Possible complications of rib fixation include dislocation and rupture of the material and infection. Reported incidence of infection is usually low (3–5%) but is of course challenging, due to the presence of the osteosynthesis material (18). Titanium is relatively resistent against infection and often allows avoiding complete removal of the material. This leads in most of the cases to keep the stability of the chest wall. The use of VAC-device is compatible with further mobilisation of the patient and long-term antibiotics are delivered.
Further development in the operation techniques should focus on minimal invasive approach. The problem in patients with flail chest is the movement of the instable segment inwards. A fixation from inside is then more physiological than from outside and should require less strength. This approach is also less traumatic for the soft tissue and reduces the risk of infection. We are developing such a minimal invasive thoracoscopic technique of fixation of the ribs.
Sternum fractures
Sternum fractures are rare (<0.5% of total bone fractures) and mainly caused by blunt anterior chest wall trauma, but also by flexion-compression injury of the trunk or by hyperextension injury tearing the sternum. Fractures mainly occur to the sternal body. Treatment is conservative in most of the cases but there is no reports assessing long-term outcome. Additionally, there is no consensus regarding the surgical approach for a sternal fracture (19). The personal experience of the surgeon in the choice of the technique is important but sternal osteosynthesis should be rigid enough to offer protection to the mediastinal structures without impairing the movement of the chest wall, in order to ensure optimal functional results and quality of life. Transverse and oblique fractures are fixed longitudinally, whereas oblique fractures of manubrium, sternocostal separation and longitudinal fractures are fixed transversally from rib to sternum to rib (20). Immediate (within 1 month after injury) indications for surgical fixation consist of emergency operation, severe or persistent pain, respiratory failure or dependency on mechanical ventilation, shifted, overlapping or impacted fractures, sternomanubrial dislocation, and hunched posture and restricted movement of the trunk. Delayed (3–6 months) indications are chronic pain, fracture nonunion or for cosmetic reason (21). Sternomanubrial dislocation is an absolute indication, since sternomanubrial joint has a protective role for the mediastinum and assists the thoracic spine in upright stability (22). Exact diagnosis is made by multi-slice CT with three-dimensional reconstruction. There are different operation techniques using steel wires, non-locking steel plates, and locked plate fixation (21). These last plates consist of different systems [fixed angle LCP plate, locked plate TiFix, low profile titanium plate 1.5 mm (MatrixRib), and SternaLock (23)]. Wires should be avoided in most of the cases due to the higher risk for secondary sternal fractures or sternal nonunion. The plates offer the advantage of a more secure reduction of the fracture with faster healing, enough rigidity and require minimal dissection of the soft tissues (24). Locked plates should be the material of choice whenever possible, since these plates have special biomechanical properties leading to reduced friction between plate and bone and to less failure. Small series have suggested that the use of titanium plates was associated with less complication, a better quality of life and is cost-effective compared to the steel plates and to the wires (22). The last improvement was introduced with the low-profile titanium plate system and the depth limited drilling to avoid injuries of the mediastinal structures. Two parallel longitudinal plates are usually placed. The technique is easy, fast and safe (24).
In summary, although management of rib fractures after stump trauma remains a controversial topic, an increasing interest for operative fixation rose in the last years. This is on one hand the result of the development of new instruments and devices allowing a quick and safe procedure and on the other hand the raising awareness in the medical community that patients can clearly benefit from an operation in selected indications in comparison with conservative therapy. It is therefore recommended to offer chest wall stabilization and rib fixation early to most flail chest patients in the absence of extended lung contusion and neurological injuries and to patients with dislocated and painful series of fractures, considering the associated injuries and the prognosis for quality of life. Surgical fixation of sternal fractures is also an underperformed procedure. Early operation in selected cases is important and required to preserve functional capacity, to prevent pseudarthrosis and chest wall deformity, and to provide good quality of life.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned and reviewed by the Section Editor Jianfei Shen, MD (Department of Cardiothoracic Surgery, Taizhou Hospital of Zhejiang Province, Wenzhou Medical University, Taizhou, China).
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/shc.2018.06.11). The author haa no conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Lardinois D, Krueger T, Dusmet M, et al. Pulmonary function testing after operative stabilisation of the chest wall for flail chest. Eur J Cardiothorac Surg 2001;20:496-501. [Crossref] [PubMed]
- Bhatnagar A, Mayberry J, Nirula R. Rib fracture fixation for flail chest: what is the benefit? J Am Coll Surg 2012;215:201-5. [Crossref] [PubMed]
- Landercasper J, Cogbill TH, Lindesmith LA. Long-term disability after flail chest injury. J Trauma 1984;24:410-4. [Crossref] [PubMed]
- Granetzny A, Abd El-Aal M, Emam E, et al. Surgical versus conservative treatment of flail chest. Evaluation of the pulmonary status. Interact Cardiovasc Thorac Surg 2005;4:583-7. [Crossref] [PubMed]
- Tanaka H, Yukioka T, Yamaguti Y, et al. Surgical stabilization of internal pneumatic stabilization? A prospective randomized study of management of severe flail chest patients. J Trauma 2002;52:727-32; discussion 732. [Crossref] [PubMed]
- Marasco SF, Davies AR, Cooper J, et al. Prospective randomized controlled trial of operative rib fixation in traumatic flail chest. J Am Coll Surg 2013;216:924-32. [Crossref] [PubMed]
- Pieracci FM, Lin Y, Rodil M, et al. A prospective, controlled clinical evaluation of surgical stabilization of severe rib fractures. J Trauma Acute Care Surg 2016;80:187-94. [Crossref] [PubMed]
- Leinicke JA, Elmore L, Freeman BD, et al. Operative management of rib fractures in the setting of flail chest: a systematic review and meta-analysis. Ann Surg 2013;258:914-21. [Crossref] [PubMed]
- Coughlin TA, Ng JW, Rollins KE, et al. Management of rib fractures in traumatic flail chest: a meta-analysis of randomised controlled trials. Bone Joint J 2016;98-B:1119-25. [Crossref] [PubMed]
- Majercik S, Cannon Q, Granger SR, et al. Long-term patient outcomes after surgical stabilization of rib fractures. Am J Surg 2014;208:88-92. [Crossref] [PubMed]
- Slobogean GP, MacPherson CA, Sun T, et al. Surgical fixation vs nonoperative management of flail chest: a meta-analysis. J Am Coll Surg 2013;216:302-11.e1. [Crossref] [PubMed]
- Kasotakis G, Hasenboehler EA, Streib EW, et al. Operative fixation of rib fractures after blunt trauma: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2017;82:618-26. [Crossref] [PubMed]
- Mouton W, Lardinois D, Furrer M, et al. Long-term follow-up of patients with operative stabilisation of a flail chest. Thorac Cardiovasc Surg 1997;45:242-4. [Crossref] [PubMed]
- Khandelwal G, Mathur RK, Shukla S, et al. A prospective single center study to assess the impact of surgical stabilization in patients with rib fracture. Int J Surg 2011;9:478-81. [Crossref] [PubMed]
- Qiu M, Shi Z, Xiao J, et al. Potential Benefits of Rib Fracture Fixation in Patients with Flail Chest and Multiple Non-flail Rib Fractures. Indian J Surg 2016;78:458-63. [Crossref] [PubMed]
- Voggenreiter G, Neudeck F, Aufmkolk M, et al. Treatment outcome of surgical thoracic wall stabilization of the unstable thorax with and without lung contusion. Unfallchirurg 1996;99:425-34. [PubMed]
- Kaplan T, Gulbahar G, Gundogdu AG, et al. An unexpected complication of titanium rib clips. Ann Thorac Surg 2014;98:2206-9. [Crossref] [PubMed]
- Thiels CA, Aho JM, Naik ND, et al. Infected hardware after surgical stabilization of rib fractures: Outcomes and management experience. J Trauma Acute Care Surg 2016;80:819-23. [Crossref] [PubMed]
- Harston A, Roberts C. Fixation of sternal fractures: a systematic review. J Trauma 2011;71:1875-9. [Crossref] [PubMed]
- Schulz-Drost S, Oppel P, Grupp S, et al. The oblique fracture of the manubrium sterni caused by a seatbelt--a rare injury? Treatment options based on the experiences gained in a level I trauma centre. Int Orthop 2016;40:791-8. [Crossref] [PubMed]
- Byun CS, Park IH, Hwang WJ, et al. Analysis of Sternal Fixation Results According to Plate Type in Sternal Fracture. Korean J Thorac Cardiovasc Surg 2016;49:361-5. [Crossref] [PubMed]
- Divisi D, Di Leonardo G, Crisci R. Surgical management of traumatic isolated sternal fracture and manubriosternal dislocation. J Trauma Acute Care Surg 2013;75:824-9. [Crossref] [PubMed]
- Chou SS, Sena MJ, Wong MS. Use of SternaLock plating system in acute treatment of unstable traumatic sternal fractures. Ann Thorac Surg 2011;91:597-9. [Crossref] [PubMed]
- Schulz-Drost S, Mauerer A, Grupp S, et al. Surgical fixation of sternal fractures: locked plate fixation by low-profile titanium plates--surgical safety through depth limited drilling. Int Orthop 2014;38:133-9. [Crossref] [PubMed]
Cite this article as: Lardinois D. General considerations, indications, and potential advantages of chest wall stabilization, rib fixation, and sternum osteosynthesis in selected patients after blunt trauma. Shanghai Chest 2018;2:62.