
Patients younger than 45 years of age have superior 5-year survival in advanced esophageal cancer
Introduction
Esophageal cancer is most frequently diagnosed in people aged 64–74, with a median age of 67 years of age at diagnosis. Patients less than 45 years of age only represent 3.2% of all patients with esophageal cancer (1). The risk factors and mechanism of disease in the young is still an area of investigation. The unanswered question remains, is the biology of esophageal cancer more aggressive when diagnosed at a younger age? Current literature on survival and characteristics of esophageal cancer comparing the young and old remains controversial. Some reports suggest that younger patients present with later stages of esophageal cancer and therefore have poorer outcomes (2,3). Others report better outcomes in the younger patients due to less co-morbidities and their ability to tolerate more aggressive treatments (4,5). The general consensus from the majority of publications is similar outcomes regardless of age (6-9). The purpose of this study is to characterize the survival of esophageal cancer in patients who were diagnosed at a young age (<45 years old) when matched with older patients who have similar stage, neoadjuvant treatment, pathology, sex, and year of diagnosis. Our hypothesis was that younger patients with esophageal cancer have a more aggressive biology and may have worse survival.
Methods
Data collection
The Mayo Clinic Institutional Review Board approved this study. A retrospective review of all patients undergoing surgical resection for esophageal cancer at the Mayo Clinic in Rochester, Minnesota between 1985–2014 was performed. Of the approximately 3,600 esophagectomies performed, only the patients under the age of 45 at the time of surgery were included in the study. During this time period similar to other publications that have examined the role of age in survival outcomes of cancer, patients were defined as young if there were 2 standard deviations below the mean age at the time of diagnosis. Therefore, the age of 45 was used as a cut off to define young patients (10,11). Patient demographics, clinical and pathologic stage, neoadjuvant and adjuvant therapy, co-morbidities, sex, history of smoking or alcohol use, and date of death were collected. Seventh edition of AJCC was used for staging.
Statistics
To assess the impact of age on outcomes of esophageal cancer, an older control group was created using frequency matching. These control patients were selected from our prospectively maintained esophageal cancer database. Patients were categorized by sex (male and female), histological subtype (adenocarcinoma and squamous cell carcinoma), age (<45 and >45 years old), pre-treatment clinical stage and neoadjuvant therapy. Year of treatment was also matched within 5 years, except for 3 cases where the matching was extended to 10 years. The potential controls (older than 45 years old) were sorted in random order and reviewed in sequence until they matched a younger (less than 45 years old patient) 1:1 by sex, neoadjuvant treatment, pathology, clinical stage, and year of surgery (12). Sex disparities in esophageal cancer were recently published from our group as a significant variable in the survival outcome of esophageal cancer (12). Neoadjuvant treatment was chosen as a matching criterion as it has been previously shown that pre-treatment does significantly affect survival outcomes of esophageal cancer (13). Lastly, surgical era was chosen as a matching criterion due to our own changes in surgical approach to esophageal cancer (1990–2005) mainly hand-sewn anastomosis vs. stapled anastomosis (2006 to present).
Categorical variables were described as frequencies (percent) and compared using Fisher’s exact test. Continuous variables were summarized using median (range) and compared using the Mann-Whitney test. Overall and disease-free survival times were calculated from date of surgery. Survival estimates were calculated using the Kaplan-Meier method, and models were created using Cox proportional hazards regression. The date of the esophagectomy was used as the starting point in the survival estimation and the date of death or last follow up was the end point. All analysis was performed using SAS, version 9.4.
Results
Patient characteristics
Eighty-two patients less than 45 years of age at time of surgery were identified. There were 69 men (84.1%), and 13 women (15.9%). Median age was 41.0 (range, 22.0–44.0) years old. The median age of the matched older patients was 66.0 (range, 51.0–81.0) years old. Co-morbidities were not prevalent in the younger than 45 group, but as expected, were significantly more common in the over 45 group. Diabetes was present in 3 patients in our younger than 45 group (3.7%), while 11 patients had diabetes in the older matched cohort (13.6%). Coronary artery disease (CAD) was present in 23.2% of the matched older patients (n=19). Smoking and alcohol use were known for 161 patients and unknown for 3 patients (1.8%). Fifty percent of young patients (n=40) were smokers, while 69.1% (n=56) of the older matched patients were smokers (P=0.0162). Alcohol use was not statistically significant between the two groups (P=0.4261) (Table 1).
Table 1
| Characteristics | Old (45+) (N=82) | Young (<45) (N=82) | Total (N=164) | P value |
|---|---|---|---|---|
| Age | <0.00011 | |||
| N | 82 | 82 | 164 | |
| Mean (SD) | 67.0 (7.7) | 39.8 (4.6) | 53.4 (15.1) | |
| Median | 66.0 | 41.0 | 47.5 | |
| Q1, Q3 | 62.0, 73.0 | 38.0, 43.0 | 41.0, 66.0 | |
| Range | 51.0–81.0 | 22.0–44.0 | 22.0–81.0 | |
| Stage, n (%) | – | |||
| 0 | 18 (22.0) | 18 (22.0) | 36 (22.0) | |
| IA | 1 (1.2) | 1 (1.2) | 2 (1.2) | |
| IB | 4 (4.9) | 4 (4.9) | 8 (4.9) | |
| IIA | 6 (7.3) | 6 (7.3) | 12 (7.3) | |
| IIB | 17 (20.7) | 17 (20.7) | 34 (20.7) | |
| IIIA | 17 (20.7) | 17 (20.7) | 34 (20.7) | |
| IIIB | 11 (13.4) | 11 (13.4) | 22 (13.4) | |
| IIIC | 7 (8.5) | 7 (8.5) | 14 (8.5) | |
| IV | 1 (1.2) | 1 (1.2) | 2 (1.2) | |
| Surgery, n (%) | 0.36212 | |||
| Ivor Lewis | 54 (65.9) | 64 (78.0) | 118 (72.0) | |
| MIE | 1 (1.2) | 0 (0.0) | 1 (0.6) | |
| McKweon | 3 (3.7) | 2 (2.4) | 5 (3.0) | |
| T.G. w/RNY | 8 (9.8) | 6 (7.3) | 14 (8.5) | |
| Trans hiatal | 16 (19.5) | 10 (12.2) | 26 (15.9) | |
| Smoking, n (%) | 0.01622 | |||
| Missing | 1 | 2 | 3 | |
| No | 25 (30.9) | 40 (50.0) | 65 (40.4) | |
| Yes | 56 (69.1) | 40 (50.0) | 96 (59.6) | |
| Alcohol use, n (%) | 0.42612 | |||
| Missing | 1 | 2 | 3 | |
| No | 44 (54.3) | 49 (61.3) | 93 (57.8) | |
| Yes | 37 (45.7) | 31 (38.8) | 68 (42.2) | |
| Diabetes, n (%) | 0.04702 | |||
| Missing | 1 | 1 | 2 | |
| No | 70 (86.4) | 78 (96.3) | 148 (91.4) | |
| Yes | 11 (13.6) | 3 (3.7) | 14 (8.6) | |
| Length of stay | 0.52941 | |||
| N | 82 | 79 | 161 | |
| Mean (SD) | 11.7 (7.5) | 10.9 (7.6) | 11.3 (7.5) | |
| Median | 9.0 | 9.0 | 9.0 | |
| Q1, Q3 | 7.0, 14.0 | 7.0, 11.0 | 7.0, 13.0 | |
| Range | 0.0–43.0 | 0.0–57.0 | 0.0–57.0 |
1, Mann-Whitney; 2, Fisher exact. MIE, minimally invasive esophagectomy; T.G. w/RNY, total gastrectomy with Roux en Y reconstruction.
In the young patient cohort, 22.0% of patients had a complete pathologic response (n=18), 6.1% had stage 1 (n=5), 28.0% had stage II (n=23), 42.7% had stage III (n=35) and only 1 patient (1.2%) had stage IV disease. We elected to match patients based on pathologic stage, thus the older matched patients had the same stage distribution of esophageal cancer (Table 1).
Surgical approach was not a variable the two cohorts were match for, thus there is some variability between the young and old groups. In both groups, Ivor Lewis esophagectomy (n=118, 72.0%) was the most common surgical approach, followed by transhiatal esophagectomy (n=26, 15.9%) (Table 1).
The overall length of stay in the hospital was not statistically significant between the two groups, median of 9 days in both groups (P=0.5294). The younger patients had no perioperative mortality, but in the matched older group, there were 2 deaths within 30 days of surgery (2.4%). In the first case, the patient had a pulseless-electrical activity (PEA) cardiac arrest on postoperative day (POD) 11 and the family withdrew care. The second patient developed a sudden headache and became unresponsive on POD 4. The patient also subsequently suffered a PEA arrest and the family withdrew care.
Survival outcomes
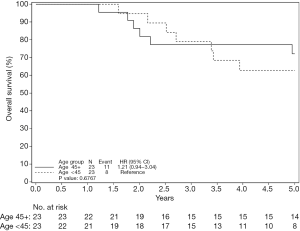
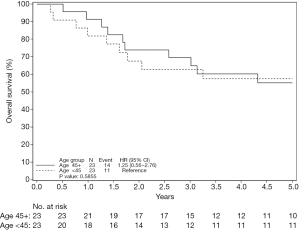
Overall survival, including all stages, was not statistically different between the <45 and match >45 groups. 1-, 3-, and 5-year survival was 89.9%, 53.7% and 44.5% in the <45 group respectively, while in the older matched cohort 1-, 3-, and 5-year survival was 79.2%, 50.2%, 39.1% (Figure 1). Overall survival by stage was also examined. Interestingly, there was no statistically significant difference in overall survival for patients aged ≥45 years relative to <45 years for either the stage I or stage II patients (Figures 2,3). However, for stage III/IV there was a statistically significant difference, where the overall survival for the younger patients was better than the match older cohort (Figure 4). 1-, 3-, and 5-year survival was 88.6%, 31.8% and 24.2% in the <45 group respectively, while in the older matched cohort 1-, 3-, and 5-year survival was 58.3%, 20.6%, 8.8% [P=0.04, hazard ratio (HR) 1.72].
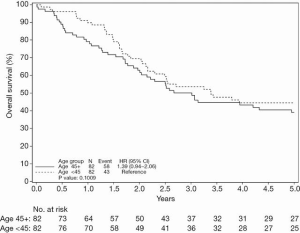
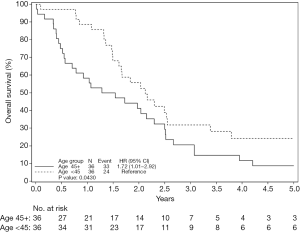
In examining the stage III/IV patient population, it was noted that the younger patients were more likely to receive adjuvant chemotherapy and radiation therapy. Sixty percent of the younger stage III patients (n=21/35) received adjuvant therapy, while only 8.6% of the older matched patients received adjuvant treatment (n=3/35) (P<0.0001, Table 2). Disease-free survival was not statistically significantly different between the two age groups regardless of stage.
Table 2
| Treatment | Old (45+) (N=82) | Young (<45) (N=82) | Total (N=164) | P value1 |
|---|---|---|---|---|
| Neoadjuvant_Chemo, n (%) | 0.7360 | |||
| No | 27 (32.9) | 24 (29.3) | 51 (31.1) | |
| Yes | 55 (67.1) | 58 (70.7) | 113 (68.9) | |
| Neoadjuvant_radiation, n (%) | 1.0000 | |||
| No | 28 (34.1) | 27 (32.9) | 55 (33.5) | |
| Yes | 54 (65.9) | 55 (67.1) | 109 (66.5) | |
| PO_Chemotherapy, n (%) | <0.0001 | |||
| No | 76 (93.8) | 40 (58.0) | 116 (77.3) | |
| Yes | 5 (6.2) | 29 (42.0) | 34 (22.7) | |
| PO_Radiation, n (%) | 0.0381 | |||
| No | 78 (96.3) | 60 (85.7) | 138 (91.4) | |
| Yes | 3 (3.7) | 10 (14.3) | 13 (8.6) |
1, Fisher exact.
Conclusions
The impact of young age on the survival, diagnosis and treatment of esophageal cancer remains an unanswered question. The overall percent of patients diagnosed with esophageal cancer under the age of 45 has been published between 3–10% (14). Early reports suggest that while younger patients have similar symptoms (dysphagia) when they develop the disease, they are less likely to seek out medical attention and therefore often present with later stages of esophageal cancer (3). A recent publication used Surveillance, Epidemiology and End Results (SEER) data to study the changes in survival, stage and age in esophageal cancer over the last 3 decades (4). They concluded, that while younger patients presented with more advanced disease, they had better overall survival. Similarly, Vallbohmer et al. found that younger patients (<50 years old) had better 5-year survival, and were receiving more neoadjuvant therapy (5). Other publications, such as Oezcelik et al. have found that younger patients are presenting at later stages and have poorer survival (3). Thus, there is no definitive conclusion in the literature regarding age of diagnosis and esophageal cancer. Importantly, the majority of publications on this topic draw conclusions based on comparisons between an older vs. young group of patients. To date, no publications have looked at the role of age on overall survival after matching patients to these significant pre-operative factors. Based on this, we chose to match patients age <45 vs. >45 with maintaining constants on stage, neoadjuvant treatment, year of surgery (within 5 years), pathology and sex.
Our retrospective review identified 82 patients from 1985 to 2014 who were diagnosed with esophageal cancer and had an esophagectomy before the age of 45. Of these 82 patients, only 9 (11.0%) were diagnosed before the year 2000. We matched these 82 patients to an older cohort of patients who had the same stage, sex, similar neoadjuvant treatment, year of surgery (within 5 years) and pathology with the primary outcome of overall survival. Our data shows that patients with stage I and II esophageal cancer have similar overall survival regardless of patient age. In contrast, we observed that younger patients had significantly better overall survival for pathological stage III/IV esophageal cancer. At 1 year the overall survival was 88.6% for the younger group compared to 58.3% in the older patient of stage III/IV patients. The 5-year survival was 24.2% in the <45 group, while in the matched group was 8.8% (P=0.04, HR 1.72). An inherent bias in the older population is a higher prevalence of co-morbidities including CAD and diabetes, that will have a significant influence on overall survival.
The most likely explanation for our finding of superior overall survival in the younger cohort with stage III/IV disease compared to the older cohort is that the younger patients were more likely to receive adjuvant therapy. Of the 35 patients with Stage III disease, 21 patients (60.0%) of the younger stage III patients received adjuvant therapy compared with only 8.6% (3/35) of the older matched patients (P<0.0001). This finding appears to be consistent with other publications that suggest that younger patients receive more treatment (surgical, chemotherapy and radiation) when compared to older patients of the same stage (5,9,10). In reviewing our charts, we found that medical oncologist and radiation oncologist were more likely to suggest adjuvant therapy because of the young age of the patient. Additionally, we also found that older patients were less likely to want additional treatment even when recommended.
We sought to answer two questions in this analysis: (I) do patients who develop esophageal cancer at a much younger age than expected demonstrate a biologically more aggressive phenotype of the disease compared to older patients? (II) Young patients diagnosed with cancer are frequently treated with much more aggressive treatment protocols primarily based on their young age. Is such a practice justified by the outcomes or is it a form of reverse ageism? Our finding that disease-free survival is not statistically significant between the two age groups, suggests that the cancer biology is likely similar regardless of age of diagnosis, and that patients who develop the disease and an unexpected young age do not appear to manifest a more aggressive phenotype of the disease. Furthermore, the more aggressive treatment strategy that is frequently employed in the younger patient cohort appears to be justified based on the superior survival results observed, particularly in those patients with more advanced stages of disease.
The question of young age as a prognostic factor has been explored in different cancer types. In breast cancer, Xiong et al. found that patients who are 30 years old or younger had a worse prognosis (15). Of importance, they found that younger patients were more likely to have estrogen receptor/progesterone receptor (ER/PR) negative breast cancer and have p53 expression, all suggestive of a more aggressive biology (15). A recent publication from Arnold et al. used the National Cancer Database to examine survival and treatment pattern in young patients with lung cancer. They found that younger patients had better overall survival, especially at the early stages (10). Additionally, the younger patients received more treatment regardless of stage.
To our knowledge, this is the only study that demonstrates the significance of age in esophageal cancer after matching patients based on significant pre-operative factors. We acknowledge several limitations of this publication. This is a retrospective study limited to one institution. Additionally, we acknowledge that matching does not completely eliminate confounding factors on survival. For example, we were not able to match on type of surgery (Ivor Lewis esophagectomy vs. transhiatal esophagectomy) and there were obvious discrepancies with co-morbidities with increased prevalence in the older population.
In conclusion, our data highlights that our younger patients have better 5-year survival at later stages of esophageal cancer when compared to older patients. Additionally, this publication highlights that as clinicians and surgeons, we tend to be more aggressive in our treatment of younger cancer patients. Overall, this survival data is encouraging especially as the number of young patients who are diagnosed with esophageal cancer seems to be increasing.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/shc.2019.07.01). KRS serves as an unpaid editorial board member of Shanghai Chest from Jul 2017 to Jun 2019. The other authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). The Mayo Clinic Institutional Review Board approved this study (No. 14-008435) and individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- American Cancer Society. Cancer Facts & Figures 2016. Atlanta, GA: American Cancer Society, 2016.
- Boys JA, Oh DS, Lewis JS, et al. Esophageal Adenocarcinoma in Patients Younger than 40 Years: A Two-Decade Experience at a Public and Private Hospital. Am Surg 2015;81:974-8. [PubMed]
- Oezcelik A, Ayazi S, DeMeester SR, et al. Adenocarcinoma of the esophagus in the young. J Gastrointest Surg 2013;17:1032-5. [Crossref] [PubMed]
- Cen P, Banki F, Cheng L, et al. Changes in age, stage distribution, and survival of patients with esophageal adenocarcinoma over three decades in the United States. Ann Surg Oncol 2012;19:1685-91. [Crossref] [PubMed]
- Vallböhmer D, Hölscher AH, Brabender J, et al. Clinicopathologic and prognostic factors of young and elderly patients with esophageal adenocarcinoma: is there really a difference? Dis Esophagus 2008;21:596-600. [Crossref] [PubMed]
- Chen H, Yang Z, Li Y. Carcinomas of the esophagus and the cardia in young patients. J Thorac Cardiovasc Surg 1994;108:512-6. [PubMed]
- Hamouda A, Forshaw M, Rohatgi A, et al. Presentation and survival of operable esophageal cancer in patients 55 years of age and below. World J Surg 2010;34:744-9. [Crossref] [PubMed]
- van Nistelrooij AM, Andrinopoulou ER, van Lanschot JJ, et al. Influence of young age on outcome after esophagectomy for cancer. World J Surg 2012;36:2612-21. [Crossref] [PubMed]
- van Nistelrooij AM, van Steenbergen LN, Spaander MC, et al. Treatment and outcome of young patients with esophageal cancer in the Netherlands. J Surg Oncol 2014;109:561-6. [Crossref] [PubMed]
- Arnold BN, Thomas DC, Rosen JE, et al. Lung Cancer in the Very Young: Treatment and Survival in the National Cancer Data Base. J Thorac Oncol 2016;11:1121-31. [Crossref] [PubMed]
- Bryant AS, Cerfolio RJ. Differences in outcomes between younger and older patients with non-small cell lung cancer. Ann Thorac Surg 2008;85:1735-9; discussion 1739.
- Rowse PG, Jaroszewski DE, Thomas M, et al. Sex Disparities After Induction Chemoradiotherapy and Esophagogastrectomy for Esophageal Cancer. Ann Thorac Surg 2017;104:1147-52. [Crossref] [PubMed]
- Donahue JM, Nichols FC, Li Z, et al. Complete pathologic response after neoadjuvant chemoradiotherapy for esophageal cancer is associated with enhanced survival. Ann Thorac Surg 2009;87:392-8; discussion 398-9. [Crossref] [PubMed]
- Donohoe CL, MacGillycuddy E, Reynolds JV. The impact of young age on outcomes in esophageal and junctional cancer. Dis Esophagus 2011;24:560-8. [Crossref] [PubMed]
- Xiong Q, Valero V, Kau V, et al. Female patients with breast carcinoma age 30 years and younger have a poor prognosis: the M.D. Anderson Cancer Center experience. Cancer 2001;92:2523-8. [Crossref] [PubMed]
Cite this article as: Saddoughi SA, Taswell J, Spears GM, Harmsen WS, Allen MS, Blackmon SH, Cassivi SD, Nichols FD 3rd, Wigle DA, Shen KR. Patients younger than 45 years of age have superior 5-year survival in advanced esophageal cancer. Shanghai Chest 2019;3:42.


